What is postpartum OCD? (And Why It’s Not What You Think)
It’s 3am. Your baby is asleep. You’ve checked on them twice already… maybe three times… just to make sure they’re still breathing. You know, rationally, that they’re fine. But you can’t shake those panic-stirring what-if thoughts. The thoughts you haven’t shared with anyone, because you feel ashamed. And so you suffer quietly, silently… alone with the terror and unsure if you’ll ever feel like the “normal” you again. If you’re a mother who sees herself in these words, keep reading…
It Might Be Postpartum OCD
Your mind feels stuck on your baby’s safety, even when there’s no clear reason to worry. Thoughts like “What if I missed something?” or “What if something bad happens and it’s my fault?” keep looping, no matter how much you try to reassure yourself.
Everything feels different in this season of life. It’s as if the volume has been turned up too loud in the scariest parts of your mind. There’s now a before and an after. You thought pregnancy would be the hardest part, and yet now you’re longing for those more carefree days when your baby was still safely nestled within. You’re grieving for a time when you didn’t feel afraid every moment of every day.
You love your baby so much it terrifies you. You want to enjoy this precious season of life with your baby, but you’re consumed by fear.
And you haven’t told anyone the full truth of what’s spiraling in your head, because you’re afraid no one will understand.
If any of this sounds familiar, I want to say something to you before we go any further:
You’re not alone. What you’re experiencing might be postpartum Obsessive-Compulsive Disorder (OCD), and it’s not your fault.
In this post, I want to help you understand what postpartum OCD actually is in real terms, not clinical ones. Why it’s so commonly missed, what keeps it going, and what actually helps to slow and stop the cycle.
Not because I read about it in a textbook. Because I’ve lived it… twice. And I know how long and slow and terrifying this season of motherhood can feel when you’re carrying this burden alone.
What is Postpartum OCD?
Postpartum OCD is an anxiety disorder that emerges in the postpartum period—typically in the weeks or months after birth, though it can also begin during pregnancy.
You might also see it referred to as perinatal OCD, which is the clinical term. “Perinatal” simply means the period surrounding birth, including both pregnancy and postpartum. In other words, perinatal OCD and postpartum OCD are describing the same condition, just at different points in the journey. I’ll use both terms interchangeably throughout this post.
Recent studies suggest that Perinatal OCD affects approximately 7.8% of women during pregnancy and 16.9% of women during the postpartum period. These numbers suggest that prenatal and postpartum OCD are much more common than originally thought. The increase in prevalence is thought to be due to the use of more comprehensive evaluation methods and a better understanding of the cluster of symptoms that define the disorder.
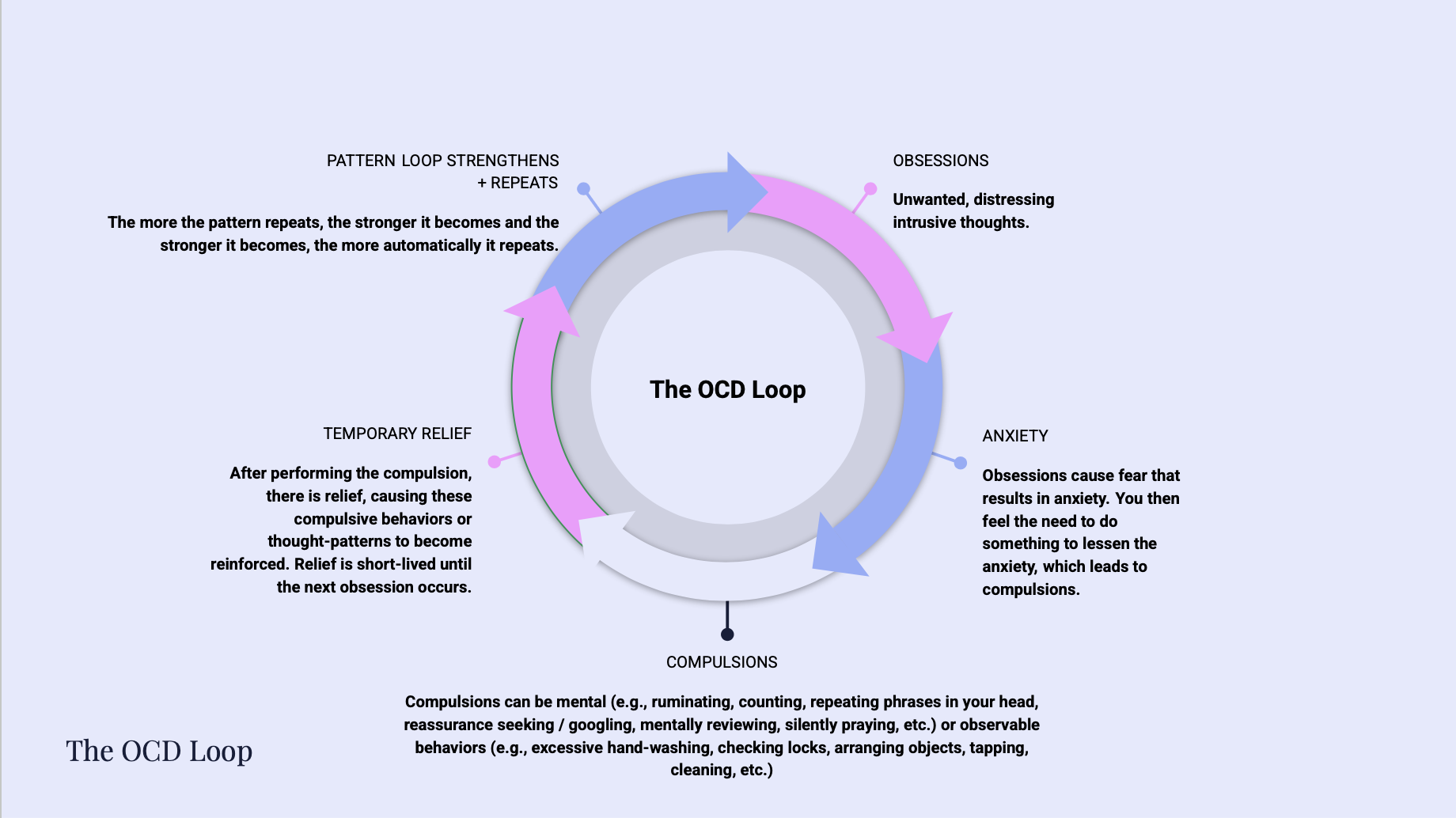
Like all forms of Obsessive-Compulsive Disorder (OCD), the postpartum OCD cycle has two primary components: obsessions and compulsions.
Obsessions
Obsessions are intrusive thoughts, images, or impulses that are unwanted and distressing. In the perinatal context, they most often revolve around the baby’s safety.
Specific obsessions in postpartum OCD might look like:
Fears of something terrible happening while you’re not watching or while someone else is caring for your baby
Fears of contamination through germs or toxins
Fears of something life-threatening or terrible being wrong with your baby
Fears of accidentally or unintentionally harming your baby
Intrusive thoughts of “losing your mind” or “going crazy” and hurting your baby
Harm-based obsessions are ego-dystonic, meaning they feel completely foreign or alien to who you are, your values, and what you genuinely want for your baby. They’re not wishes, they’re not desires or urges that you secretly want to act on. They’re the opposite. They’re intrusions that horrify you precisely because they contradict everything you actually feel about your baby.
Compulsions
Compulsions are the responses (behaviors, mental rituals, or reassurance-seeking thought loops) that are performed in hopes of reducing the fear that the obsessions create. Compulsions may provide temporary relief, but they create long-term anxiety and feed the OCD cycle.
If an obsession is the fire, then a compulsion in response is the fuel.
Specific compulsions in postpartum OCD might look like:
Waking in a panic at 3am (again) to make sure your baby’s still breathing
Googling symptoms or seeking reassurance (hello, babycenter forum... we meet yet again) to feel certain you haven’t missed something—”Was that funny movement she just made a normal reflex or is something seriously wrong with her?”
Asking doctors, experts, other mothers, or your partner for reassurance that your baby is okay / normal / healthy
Confessing your intrusive thoughts to someone else to make sure you’re still a good person and a good mother
Comparing your baby’s “stats” (e.g., head circumference, weight, height, etc.) to growth charts to “make sure” everything is normal
Overanalyzing your baby’s bowel movements, reflux, feeding schedule, and milestones and feeling panicked about anything slightly out of the ordinary
Mentally reviewing interactions or decisions to make sure you didn’t make a mistake
Avoiding situations, people, or places that feel even slightly risky to your baby’s safety
Going to extreme lengths to protect your baby from contaminants (e.g., germs and/or toxins)—for example, not allowing others to hold your baby or having very strict rules around others holding your baby
Ruminating about your baby’s health, safety, or well-being
Many mothers don’t recognize these behaviors or thought loops as compulsions and initially dismiss them as reasonable responses to genuine fears. This is part of what makes postpartum OCD so difficult to identify early on. This is especially true if your compulsions are solely or primarily thought-based (i.e., rumination).
However, the more the cycle repeats, the deeper and more anxiety producing it becomes. What was once dismissed as “typical new-mom fears” spirals into a painful, all-consuming, unstoppable cycle of terror that shrinks your world smaller and smaller.
The OCD Loop
What Postpartum OCD Actually Looks Like
Because postpartum OCD is so widely misunderstood, many mothers spend months (or even years) without having a name for what they’re experiencing. They might sense they’re struggling with Postpartum Anxiety (perhaps their doctor has even diagnosed them with it), yet there’s this looming sense that what they’re experiencing goes beyond anxiety.
Here is what Postpartum OCD can look like from the inside:
Intrusive images of harm coming to your baby, whether by accident, by illness, or by your own hands. These thoughts arrive uninvited and feel impossible to shake.
A terror of being alone with your baby that you can’t explain or justify to anyone, including yourself. This can be especially confusing if you’re also afraid of leaving your baby alone with anyone else, because you’re both triggered by your baby’s presence and by their absence.
Checking rituals that provide a very brief period of relief (seconds, minutes, or hours) before the fear returns, strong than before
Hours of googling or searching on forums, looking for evidence that the scary what-if thought is inaccurate, wrong, or unlikely. With OCD though, even “unlikely” isn’t good enough. OCD demands certainty. 100% certainty that nothing bad will ever happen to your precious baby.
A running mental film reel of worst-case scenarios that you can’t turn off
Feeling exhausted and yet hypervigilant at the same time—as if you’re trying to move through life by slamming on both the gas pedal and the brake pedal at the same time.
Feeling incredibly lonely, isolated, different, “wrong”, broken, crazy. You don’t want to carry this burden of terror alone and yet you’re scared what someone would think or do if they knew what you were going through inside.
Postpartum OCD looks different for every mother. Some are primarily checkers. Some are caught in mental loops (rumination) of reviewing and attempting to solve. Some are mostly focused on avoiding. Many women do all three.
Regardless of what the specifics of the obsessions and compulsions look like, the OCD cycle is the same for all mothers. And often, the silence and isolation is too.
Why Postpartum OCD is Commonly Missed
For a condition that affects so many mothers, postpartum OCD is remarkably under-identified. There are a few reasons for this…
It doesn’t look the way people expect OCD to look. Most people’s image of OCD involves hand-washing, counting, or symmetry. In reality, OCD (whether traditional, prenatal, or postpartum) often looks very different than this, and the symptoms can be hidden or invisible to outsiders. In the case of postpartum OCD, it often looks like a devoted, terrified mother doing everything she can to keep her baby safe. From the outside, she often appears to be an anxious yet highly attentive parent. The internal experience, though, is entirely different. It’s painful, exhausting, dark, tormenting, and isolating. It feels like playing a never-ending game of whack-a-mole with new fears constantly popping up.
She’s hiding it. The intrusive thoughts that initiate the OCD cycle can be incredibly contradictory to what a “good mother” is supposed to think and feel. The anxiety and terror and grieving for the mental freedom she had before her baby was born can also induce feelings of shame… as if she’s a bad mother for not enjoying this precious season of life. Mothers struggling with postpartum OCD often fear being judged. They fear being labeled as dangerous or unfit to parent. Because of this, they carry the burden alone… silently suffering while doing their best to show up as the mother they know they are beneath the terror.
It’s confused with other postpartum conditions. Standard postpartum mental health screenings, including those used for both postpartum depression and postpartum anxiety, don’t reliably capture OCD presentations. While postpartum OCD does fall under the broader umbrella of postpartum anxiety, OCD is a separate and distinct disorder with a specific presentation that requires a tailored treatment approach. Many mothers receive support for anxiety and/or depression that helps partially, but fails to address the underlying roots that keep the OCD cycle alive.
The result = a mother who is suffering deeply, trying hard, holding everything together on the outside yet feeling completely alone with what’s happening on the inside. She deserves better than that, and she needs more than that to recover.
What Keeps the OCD Cycle Going
Whatever you’re doing to feel better in the short-term are the very things that are keeping the OCD cycle alive long-term. This is true whether it’s checking, googling, seek reassurance from doctors and experts, or ruminating.
The Cycle
A distressing intrusive thought arrives → fear spikes → you perform a compulsion (e.g., check, google, seek reassurance, ruminate, avoid, etc.) → fear temporarily reduces and you feel relief → then, minutes or hours later, the intrusive thought returns louder and stronger than before (or a new, even scarier thought emerges in its place) → the cycle repeats
The thing is that every time you respond to the thought with a compulsion, you send a signal to your nervous system. One that says: this threat is real and important and requires your response. The intrusive thought gets moved up the priority list every time it’s responded to as a real threat.
Your brain and nervous system are doing their jobs perfectly, and every time the OCD cycle repeats, it also strengthens, deepens, and becomes “stickier”. Because neurons that fire together, wire together. And the OCD cycle becomes more entrenched in the brain and nervous system through repetition.
Here’s What You Need to Know
Compulsions will almost always provide some degree of short-term relief, which is what makes them so sticky, so self-sustaining, and so enticing. It’s the relief the compulsion provides that trains you to take the fear-bait and repeat the compulsion in reaction to the obsession again in the future.
This isn’t your fault. You’re not weak for giving into compulsions. In fact, without understanding how the cycle works, it makes perfect sense to give in because giving in provides immediate relief and that’s what the brain remembers. That’s the memory of the compulsion that becomes imprinted in the subconscious mind. Compulsion = relief. Unfortunately, this isn’t the whole picture.
What doesn’t get imprinted into the subconscious are the broader, long-term consequences of the cycle. What doesn’t get imprinted is this…
Compulsion = relief now and stronger OCD cycle later
The subconscious memorizes emotions with keen precision (especially when it comes to moving us away from pain and towards pleasure), but it’s not able to discern the long-term emotional outcomes of patterns. It memorizes immediate cause-and-effect sequences.
This is why whatever the subconscious memorizes as providing in-the-moment relief is remembered and repeated every time the same pattern of pain emerges. And it’s this knee-jerk subconscious reaction that’s responsible for that nearly irresistible urge-y feeling that pushes us to engage in a compulsion. The subconsciously driven promise of relief when we’re feeling terrified is why it can feel almost impossible to say “no” at this point in the cycle.
This is why we often know better yet struggle to do better. The subconscious mind is responsible for about 95% of what we do, think, and feel. And it runs those thoughts, actions, and feelings on autopilot.
With the OCD cycle, the subconscious mind has “jumped the shark” so to speak and linked compulsions with relief without recognizing that the relief is incredibly short-lived and is, in fact, the cause of long-term pain.
Here’s what’s imperative to remember…
When it comes to OCD, short-term relief always strengthens long-term anxiety. Yes, always.
This is the part that changed everything for me when I finally understood it. And it’s the part I want you to hold onto.
Anything you do (whether physically or mentally) to alleviate fear now will strengthen fear later. Stated more simply, anything you do to feel better now (e.g., checking, googling, ruminating, reviewing, reassurance-seeking, etc.) will will strengthen the OCD cycle and make you feel worse later.
It’s a frustrating and uncomfortable truth to embrace, but it’s the truth. I’ve lived it, I’ve been there… the only way out is through. Sitting with the discomfort until the fear plateaus and eventually falls.
Knowing this is the key to choosing best and better for yourself going forward. Because this point—the one that exists between obsession and compulsion—is our only point of choice in the cycle. We can’t choose to stop intrusive thoughts from coming in. Thought stopping doesn’t work, at least not with OCD. However, we can choose to stop engaging in compulsions.
Here’s the tricky part though… initially, it will feel irresponsible to not engage in compulsions. Here’s why…
How Shame Factors Into the OCD Cycle
The driving force behind the OCD cycle (in both traditional OCD and postpartum OCD) is an intolerance to uncertainty. This is why it’s often referred to as “the doubting disease”. In the case of postpartum OCD, it’s an intolerance to the discomfort of anything (real or imagined) that could potentially threaten the well-being and safety of your baby.
It’s also a fear of not being responsible enough or thorough enough to protect your baby from everything and anything that could possibly bring her harm.
And this is where shame seeps into the OCD cycle and helps sustain its hold. Because shame will make you feel irresponsible for not responding to the obsessions with compulsions. When the fear of the intrusive thought isn’t enough to get you to react, OCD uses shame to up the ante.
Shame will attempt to convince you that you’re a bad mother if you don’t engage in compulsions… if you don’t check… if you don’t “make sure just one more time”…. if you don’t treat that what-if intrusive thought as a real threat.
This is where postpartum OCD can become so sticky. Because it uses shame to attack your character, your integrity, your responsible nature. And the energy of shame feels terrible… especially when it targets our worth or goodness as parents. We’ll do anything we can to avoid feeling shame, including continuing to engage in the very compulsions that keep the painful OCD cycle alive.
Because it feels irresponsible as a mother to not check. To not make sure. To not overprotect, verify, and guard our precious, innocent, everything baby.
I promise you this, though…
Shame is a liar. It’s a façade… a wall, a fence, a gate. It’s terrifying, yes. It feels heavy, palpable, viscerally uncomfortable… nauseating even. Which is why we so often treat it as a “do not enter” sign when it comes to our own emotional terrain.
Here’s What Helps
Recovery from postpartum OCD is real. I know this, because I’ve lived it. And I’ve spent nearly a decade studying the ins and outs of OCD and becoming a so-called guinea pig to discover what works and what doesn’t. I did this to help myself, yes, and I also did it for mothers like you. I did it with the long-term hope of eventually, someday, guiding other mothers out of the darkness too.
Exposure and Response Prevention (ERP)
Exposure and Response Prevention (ERP) is considered the gold standard treatment for OCD, and for good reason. In ERP, you gradually face the feared thought or situation without performing the usual compulsive response.
Over time, this teaches the nervous system that the thought is not a threat. It also teaches you that you can tolerate the discomfort of fear without needing the crutch of the compulsion to alleviate it. Over time, the relief that used to require checking, googling, or reassurance-seeking becomes available by simply staying present for the rise, plateau, and eventual fall of fear.
ERP is effective, and if you have access to an OCD-specialized therapist who offers it, it is worth pursuing. Its limit though is that it addresses the cycle but fails to reach the root cause beliefs driving the cycle. Because of this, the fear tends to keep finding new forms, new targets, new ways in. With ERP, the surface-level cycle is treated but the underlying core wound or fear isn’t.
Nervous System Regulation + Somatic Work
A dysregulated nervous system makes everything harder, including ERP. Building a daily body-based regulation practice alongside the cognitive work creates the neurological conditions for deeper healing. When the nervous system is calmer at baseline, the intrusive thoughts have less power and literally feel less scary than when the nervous system is in survival mode. From a state of regulation, the spike of fear from the intrusive thought is less threatening and we have a more accurate assessment of our own resilience. In other words, it’s easy to brush the once terrifying thought off with a simple, “Maybe that will happen… maybe it won’t… I’m going to keep on living my life here and now, because that’s where my point of power is.”
In a state of regulation, the window or gap between the intrusive thought and the compulsion is also wider, reducing the feeling of urgency and making it easier to resist the compulsion rather than engage it.
Root Cause Work
This what I’ve built my practice around after living through postpartum OCD twice and experiencing a relapse in perimenopause. I tried everything I possibly could to get better…
I tried CBT. I tried mindfulness. I tried medication. I tried meditation. I tried EFT. I tried herbs and supplements. I tried tinctures. I tried quantum healing. I tried reiki. I tried special elimination diets. I tried ERP… twice.
It all helped… for a while. But the fear kept finding new forms, new targets, new ways in. Because the work addressed the surface-level symptoms rather than the core wound behind them.
Trying to address the specific fears one at a time felt like playing a game of whack-a-mole I’d never win… there was always a new fear, always a new way for OCD to take hold. One fear would be resolved only for another to quickly take its place.
Once I began to study the subconscious mind, I realized that I didn’t need to understand the specific contents of the OCD fears better… I needed to understand the root cause that was driving them. I needed to understand the subconscious core wound underneath all the scary thoughts.
Because it was that core wound (in my case, the fear of being left behind due to my own negligence) that continuously fueled the cycle, and it was resolving the core wound at a subconscious level that finally created lasting change. This is why root cause work is at the center of The 4R™ Method I’ve created to support mothers in recovering from postpartum OCD and returning to their lives stronger and more resilient than ever.
If you’re curious about what this approach to recovery looks like, you can learn more about it here.
You Don’t Have to Keep Carrying this Alone
If you’ve made it this far, I want you to know something: the fact that you’re here, reading this, trying to understand what’s happening… that is one of most loving things you can do for yourself right now. Awareness opens the path to healing.
Postpartum OCD isn’t who you are. It’s a cycle—a painful pattern masquerading as a relieving one—that’s unfolding within you in a season of extraordinary neurological, physical, and emotional demand. This cycle has a name, it has a map, and it has a way out.
If you’re ready to talk or looking for more support, you can learn more about how I work with mothers navigating postpartum OCD by scheduling a free 30-minute consultation, learning more about my background and training on Psychology Today, or listening to my podcast (The Soul Horizon) on Spotify or Apple Podcasts.
Sources
https://perc.psychiatry.uw.edu/wp-content/uploads/2025/06/Perinatal-OCD-Care-Guide.pdf